
Patients with heart rhythm problems (specifically atrial fibrillation) are using a mobile phone app to remotely monitor their heart rate and rhythm and avoid in-hospital appointments during the COVID-19 pandemic.
Caring Futures Institute researcher and Leo J Maher Cardiovascular Nursing Chair Dr Jeroen Hendriks has been working with Associate Professor Dominik Linz and Nikki Pluymaekers from Maastricht University Medical Centre+ in the Netherlands on the rapid implementation of the mobile health (mHealth) application, known as the TeleCheck-AF project.
Patients are prescribed the mHealth app, called FibriCheck, to measure their heart rate and rhythm seven days before engaging in a teleconsultation with a health care professional.
Patients record three measures a day and provide data on vital parameters that are important to evaluate and maintain treatment.
As such, patients are actively involved in their care process and contribute to their own health outcomes. After a week of readings, they have a telehealth consultation with their health care professional who will analyse the data and advise accordingly.
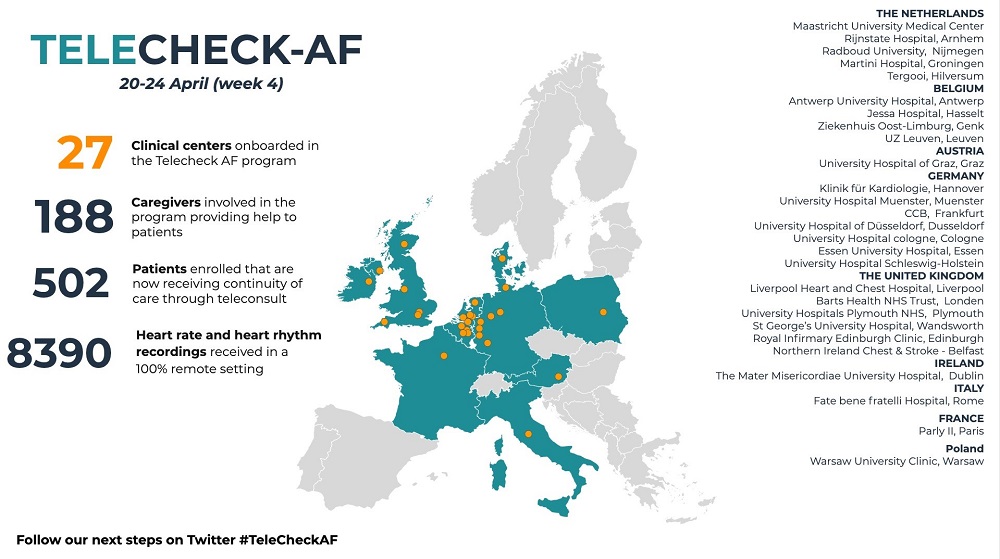
The implementation of this project started four weeks ago in the Maastricht centre and already 27 centres across nine European countries are involved, with 500 patients using the application.
Cardiologists and specialised AF nurses at the Maastricht’s cardiology department are using the app to track the heart rhythm and rate of patients with atrial fibrillation – irregular heartbeat – so patients can avoid visiting the hospital for an ECG during the COVID-19 pandemic.
The app records a pulse when the patient places their index finger over the camera on their smartphone for one minute to measure their heart rhythm. An algorithm then identifies if the patient has a heart rhythm disorder or is in the normal rhythm (sinus rhythm) and if their heart rate is too fast or too slow.
After a week of readings, the patient has a telehealth consultation with their health care professional who will analyse the data and advise accordingly.
Dr Hendriks says the benefits of the project included reduced risk of COVID-19 infection and patients have an active role in their treatment.
“The benefits of this approach is that patients don’t have to come to the hospital which reduces the risk of COVID-19 infection,” he says.
“Also, activating patients in their role to perform the measures may lead to improved involvement in their treatment and consequently improved adherence to the treatment regimen and lifestyle management.
Dr Hendriks says the response from patients so far has been “very positive” and that the TeleCheck-AF approach and use of the technology is here to stay.
“The TeleCheck-AF approach as well as the use of the technology will continue after COVID-19,” he says.
“One of the advantages may be that there is reduced care utilisation which may reduce the burden of the health care system. However, it is too early to draw conclusions and currently research projects are being prepared.
“Nevertheless, this approach will not replace the traditional outpatient consultations, so that those patients who don’t use a mobile phone or not that mHealth savvy can still receive their care as usual.”
For more information visit the website www.telecheck-af.com or check out the #TeleCheckAF hashtag on Twitter.

