
Why Regional Health? What a trip!
Who would have thought, when I commenced physiotherapy studies at the University of Adelaide in 1961, that I would become so passionate about health inequalities? Particularly the health of children and families.
Working as an aide in the physiotherapy department of the Adelaide Children’s Hospital (now the Women’s and Children’s Hospital), towards the end of the second large polio epidemic, many of our patients were country children. Some came from the Northern Territory; many came from outer regions and remote areas of South Australia. Most of these children spent many months in Adelaide, in hospital or in Estcourt House, a rehabilitation establishment, learning to manage their resultant disability, before their return to their home communities. I think this is where I first developed some understanding of the isolation of distance when specialized management is required.
Several years later, following teaching and practicing paediatric physiotherapy in Adelaide, our family, now General Practitioner husband and two small children, went to the north coast of Papua New Guinea to live and work. Here I learnt so much about communities, acceptance and endeavour. No more the quick telephone call seeking advice or confirmation, our patients needed help and they needed it NOW. I remembered the old advice of our family paediatrician when I sought his support on my intentions to commence private practice: “First of all, do no harm”. With his words ringing in our ears, we learnt to adapt treatment and advice to the needs and beliefs of the village people with whom we were dealing. We learnt to listen to their beliefs and wishes for their health, to adapt our programmes to suit their environment and traditions. We learnt to communicate in Pidgin English – a universal language in PNG. Pidgin uses simplistic descriptive language to enhance comprehension, what better way to communicate health education and advice to people!
We returned to South Australia when the struggle for Independence in PNG was growing and although locally there was little effect, there was a growing fear of how this would develop over the ensuing years. We left with nothing but love for the country and its people and a feeling that capital city living was not for us.
We accepted a position in regional South Australia, in Mount Gambier, where Peter could continue procedural general practice, as we anticipated the arrival of our third child. My job was to settle our young family in the new environment and establish our home there as Peter’s workload increased. The pace of living was different here, as was the work expectation. There was, however, a strong feeling of community with loyalty to local endeavour, but opposition from some to me working.
Overcoming the battles of recognition as a physiotherapist with paediatric and teaching capabilities introduced me to the need to demonstrate the advantages of local availability and knowledge to regional health. Clinical placement opportunities were created, not only with physiotherapy students but also with many of the medical students who stayed in our house while learning first-hand about the life of a rural/regional doctor. My teaching appetite was whetted again.
A particular interest developed in the apparent differing outcomes for rural/regional children with disability and their metropolitan counterparts.
 I was increasingly disturbed by the discrepancy in outcome for children with developmental dysplasia of the hip (DDH) or foot deformities such as talipes equino-varus (club foot). Such children often had a worse outcome than their city counterparts.
I was increasingly disturbed by the discrepancy in outcome for children with developmental dysplasia of the hip (DDH) or foot deformities such as talipes equino-varus (club foot). Such children often had a worse outcome than their city counterparts.
Development of the Greater Green Triangle University Department of Rural Health, a joint endeavour of Flinders and Deakin Universities, presented a life-changing opportunity for me to amalgamate my clinical, teaching and regional experience with some credible research. I began to explore any recognised clinical differences in outcome for regional children and what might be causative if this were the case. I received two grants to explore any differences in diagnosis and management of infant hips, but although there was local interest, there seemed little central interest in these regional findings.
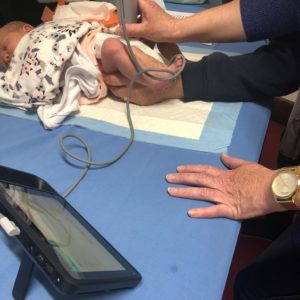
(image : is a shot of a 10 day old baby having a hip scan in my rooms. It shows the portable ultrasound and the way in which the hips are scanned to measure any instability. Tailored advice can then be offered to the parents on hip care and management. This service is offered to all families with children born at the regional hospital if they wish to come to have it done in the first two weeks after birth.)
The expansion and development of the Flinders University Rural Clinical School presented an opportunity for me to continue my studies by acceptance into a doctoral programme. I was unaware of the possibility of remote learning at this level. The advice and support from Flinders University was exceptional. I was able to continue my study of Early dynamic ultrasound in the assessment and management of neonatal instability of the hip, the topic of my doctoral study, receiving my doctorate at the end of 2019.
Perhaps one of my regrets is that I did not embrace Flinders University opportunities as fully as I could have in the early months. I think the surprise of being accepted into the programme, together with my strong, independent nature, led me to believe that if there were faith shown in my abilities, I needed to demonstrate my ability to complete the task. I would strongly advise students embarking on distance education such as this to make early contact with the Office of Graduate Research and learn first-hand, what opportunities are available. I believe that a week of familiarization with the opportunities available on campus, meeting with a librarian and other experts in the field, would have been beneficial to me. This was my first experience of serious digital learning and I had much to learn about digital techniques and remote learning. Flinders University offers a wide range of supports for its students, if only I had realized this at the beginning. When I did visit the campus at Bedford Park, I felt overwhelmed by the young vibrant students around me. They all apparently knew where they were going and what they were doing. Getting to Adelaide not only involved a lengthy road trip, it was necessary to make arrangements for days away from home and work, not always easy with a busy GP husband and family at home.
My family was extremely proud of what I was doing and quickly understood that “Mum was studying”. They were extremely useful as they endeavoured to help me develop my computer skills. They have shared so much in the growth and development of my study. I became more confident in seeking and sourcing help, accessing programmes on iEnrol and tailoring visits to include several training sessions.
Flinders University presents a wonderful and supportive environment in which to continue my study. An introduction to the Write Bunch provided great peer support and expanded my writing. In particular, the support of the Dean and the Office of Graduate Research empowered me to disseminate the findings of my research and continue the discussion.
But, the research did far more than that! It unexpectedly highlighted inequalities in regional health, digital literacy and health education between different regions. It accentuated the somewhat transient nature of health employment, the difficulty of continuing professional development, mentoring and State Borders together with the funding diversity between State and Commonwealth. Who knew that it would be such a complex field?
All these complexities have been further compounded by the effects of the current corona- virus, Covid19, sweeping the World. Recognition of this led to my recent publication in Social Alternatives vol. 39 no.2, published recently. The inability to move between States has imposed severe restrictions on specialist and locum visits to fill gaps in rural and regional centres. Combined with increasing guidelines for evacuation of patients to capital cities for treatment and a lack of commercial airline travel, a much-increased difficulty in regional patients accessing vital treatment has been seen. Discussion and action must be taken to ensure that regional communities are able to manage more complex situations closer to home.

